
Spine Surgery
- Show All
-
Back health
-
lower back pain
-
Treatments
-
Lumbar Spinal Stenosis
-
sciatica
-
Spine conditions
-
Lumbar Pain
-
spinal stenosis

How do I Care for Myself at Home After My Spinal Surgery?
Patients scheduled for back surgery are rightfully concerned about their recuperation and how t...

Preparing for Spinal Surgery
Whether to treat a slipped disc from age-related spinal degeneration or a traumatic spinal ...

Spinal Surgery for a Slipped Disc
Each year, for every 1,000 adults, there are approximately 5 to 20 cases of disc herniation. Al...

Caring for Your Spinal Surgery Incision
All patients undergoing back surgery should actively ensure that the healing process goes a...

How to Prepare for Spinal Fusion Back Surgery?
Spinal fusion is often performed in conjunction with spinal decompression surgery for vario...

What is Lumbar Spinal Stenosis?
Spinal stenosis is a prevalent spinal disorder in the U.S. and across the globe. In fact, the c...

Is There a Cure for Lower Back Pain?
Lower back pain is among the most common medical problems affecting the human population. O...

What is Endoscopic Spine Surgery?
The last several years have seen great strides in developing advanced surgical solutions for sp...

What is a Lumbar Laminectomy?
Medical terminology doesn’t go out of its way to be complicated or hard to understand. It’s...

Motion Preservation Surgery in The Lumbar Regions of The Spine
The lumbar region of the spine is the most susceptible to pain and injury. This is due to its m...

What is Spondylolisthesis?
If you’re struggling with persistent back pain along with numbness, tingling, or weakness, ...

What is Laminoplasty?
Spinal stenosis is a prevalent spinal condition that can cause neck or back pain and neurologi...

What is Lumbar Spinal Fusion?
Chronic lower back pain is an extremely common medical issue across the world. In a study condu...

Can You Get Blood Clots From Spinal Surgery?
Spinal surgery has made significant advances in both its safety and efficiency in correctin...

How much physical therapy do I need after spinal surgery?
Whether a patient is having open back surgery for a spinal cord injury or a minimally invasive...

Are some spinal surgeries more successful than others?
Are some spinal surgeries more successful than others? The short answer is yes, but that ...

Causes of Back Pain in Adolescents vs. Adults
Though the majority of spinal problems appear between the ages of 35 and 55, wrought by nat...

What Is XLIF?
Thanks to breakthroughs in spinal medicine, patients today can benefit from treatment regimens ...

Why are some spinal surgeons more successful than others?
It’s a fact that some spine surgeonshave higher success rates for the operations they per...

Choosing a Spinal Surgeon
Choosing a spinal surgeon is among the most important medical decisions a patient can make. A ...

Advantages of Medical Tourism
Can you really travel to a foreign destination for a vacation and receive high-quality medical...

How soon can you return to athletics after spinal surgery?
Near the top of the list of questions from almost every spinal surgery, the patients indica...

Taking Vitamins Before Surgery
Spinal surgery is stressful on the body. Anyone who is having spine surgery needs to prepare h...

Should I stop taking medications before spinal surgery?
You have a pinched nerve, slipped disc, a spinal cord injury, or other back problem that ...

What should I expect the day of my spinal surgery?
This is the big day, the day your spinal surgery will be performed and your back condition – b...

Post Op Day 1
You had your back surgery operation yesterday. The day after a lumbar laminectomy, spinal...

Recognizing and Preventing Post-Surgical Complications
With advanced procedures performed by highly trained and experienced surgeons, spinal surgery t...

What is Claudication?
Its name sounds complex, but the condition is very basic: Claudication is a pain, typically in...

Post Op Day 2
You had spinal surgery two days ago – perhaps it was for a simple but persistent pinched ...

What is Neural Claudication?
Recently, we addressed the topic of claudication. Claudication refers to pain typically felt in...

What is Radiculopathy?
Have you heard of radiculopathy? This condition results from nerve irritation and, if it progre...

What is Lumbar Radiculopathy?
The human body contains an extensive system of nerves that facilitate communication between th...
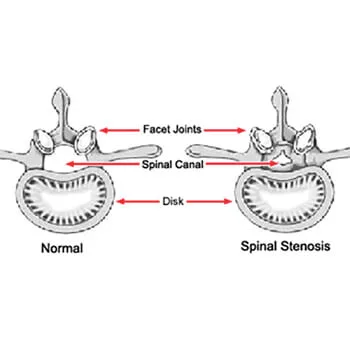
What is Lumbar Spinal Decompression?
Lower back pain has long been a prevalent health concern around the world. In 2017, the preval...

Back Treatment Options
In our previous blog we discussed the tremendous stresses borne by the lumbar, or lower portio...

Preparing for Spinal Fusion Surgery, Part II
In our last blog we began addressing the topic of preparing for spinal fusion back surger...

How Soon Can I Get Out of Bed After Spinal Fusion Surgery?
We’ve addressed preparations for back surgery in recent blogs and specifically the surgery ...

What is Failed Back Surgery Syndrome?
Failed back surgery syndrome (also called FBSS, or failed back syndrome) is a generalized t...

Common Questions About Back Pain: Do You Need Back Surgery?
Back pain affects an estimated eight out of 10 people over the course of their lives. So, it’s...

Common Questions About Back Pain: What are the Different Types of Back Surgery
There are several different types of back surgery proving successful at resolving patients’ ba...

