
Treatments
- Show All
-
Back health
-
lower back pain
-
Treatments
-
Lumbar Spinal Stenosis
-
sciatica
-
Spine conditions
-
Lumbar Pain
-
spinal stenosis

Treatment of Lumbar Spinal Stenosis
It’s common for office and remote workers to suffer from back pain, and some of them even consi...

How do I Care for Myself at Home After My Spinal Surgery?
Patients scheduled for back surgery are rightfully concerned about their recuperation and how t...

Types of Back Pain
Back pain is one of the most complex and confounding conditions in medicine. There are seve...

Is There a Cure for Lower Back Pain?
Lower back pain is among the most common medical problems affecting the human population. O...

What is a Lumbar Laminectomy?
Medical terminology doesn’t go out of its way to be complicated or hard to understand. It’s...

Reuters reports on Premia Spine’s TOPS System and farmer Yehuda Schwartz
https://www.youtube.com/watch?v=W7fGA38jpx4

What Is Sciatica?
Everyone has heard of sciatica, but few people know what it actually is – or isn’t. Sciatic...

What is Spondylolysis?
Although it’s not as common as spinal stenosis or a herniated disc, spondylolysis is near the ...

What is Lumbar Radiculopathy?
The human body contains an extensive system of nerves that facilitate communication between th...
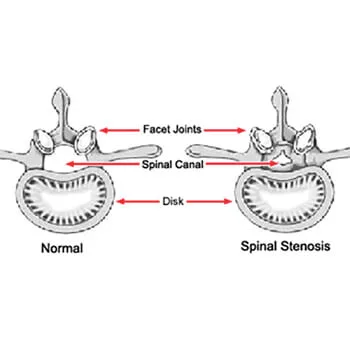
What is Lumbar Spinal Decompression?
Lower back pain has long been a prevalent health concern around the world. In 2017, the preval...

Back Treatment Options
In our previous blog we discussed the tremendous stresses borne by the lumbar, or lower portio...

Back Pain and Steroid Injections
Epidural injections of steroids have often been the treatment of choice for patients with ...

What Is Back Strain? Symptoms, Causes, Treatment of Back Strains
Though it’s commonly played down, a back strain can be an extremely painful and demobilizin...

Common Questions About Back Pain: What are the Different Types of Back Surgery
There are several different types of back surgery proving successful at resolving patients’ ba...

