
Lumbar Spinal Stenosis
- Show All
-
Back health
-
lower back pain
-
Treatments
-
Lumbar Spinal Stenosis
-
sciatica
-
Spine conditions
-
Lumbar Pain
-
spinal stenosis

Lumbar Spinal-Lateral Recess Stenosis
Lumbar spinal-lateral recess stenosis is a type of spinal stenosis involving the narrowing of t...

Lumbar Foraminal Stenosis
The spine is made up of various structures, including the foramina. These openings in the verte...

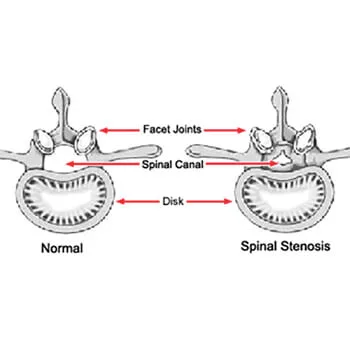
What is Lumbar Spinal Stenosis?
Spinal stenosis is a prevalent spinal disorder in the U.S. and across the globe. In fact, the c...

Lumbar Stenosis with Neurogenic Claudication
The spine is one of the most important elements of the human body. When it stops working proper...

What is the X-Stop procedure?
X-Stop is a minimally invasive spinal surgery procedure that may be performed to treat cases o...

Why are some spinal surgeons more successful than others?
It’s a fact that some spine surgeonshave higher success rates for the operations they per...

Choosing a Spinal Surgeon
Choosing a spinal surgeon is among the most important medical decisions a patient can make. A ...

How soon can you return to athletics after spinal surgery?
Near the top of the list of questions from almost every spinal surgery, the patients indica...

Should I stop taking medications before spinal surgery?
You have a pinched nerve, slipped disc, a spinal cord injury, or other back problem that ...

What is Neural Claudication?
Recently, we addressed the topic of claudication. Claudication refers to pain typically felt in...
What is Lumbar Spinal Decompression?
Lower back pain has long been a prevalent health concern around the world. In 2017, the preval...

Back Treatment Options
In our previous blog we discussed the tremendous stresses borne by the lumbar, or lower portio...

Back Pain and Steroid Injections
Epidural injections of steroids have often been the treatment of choice for patients with ...

Preparing for Spinal Fusion Surgery, Part II
In our last blog we began addressing the topic of preparing for spinal fusion back surger...

How to Prepare for Spinal Stenosis Surgery, Part III
Spinal stenosis, an unnatural narrowing (or stenosis) of the spinal canal, is an all t...

How Soon Can I Get Out of Bed After Spinal Fusion Surgery?
We’ve addressed preparations for back surgery in recent blogs and specifically the surgery ...

