What is Spondylolisthesis?
If you’re struggling with persistent back pain along with numbness, tingling, or weakness, you may have a spinal condition. Spondylolisthesis is one possible condition that can trigger these symptoms and ultimately compromise your quality of life.
In this article, we’ll dive into the topic of spondylolisthesis and explain what patients can expect from a spondylolisthesis diagnosis. While the prospect of managing this condition may seem intimidating, rest assured that there are numerous effective treatment options for spondylolisthesis.
What is Spondylolisthesis?
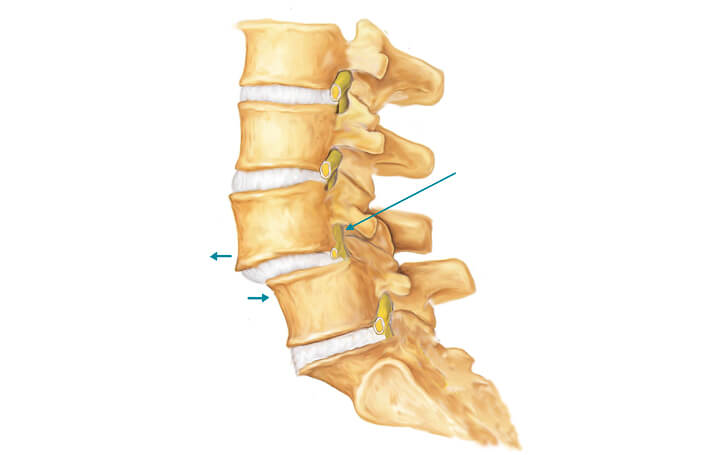
With spondylolisthesis, one of the vertebrae in the spine becomes displaced due to instability. As a result, it moves downward in relation to its proper position, settling on the vertebra beneath it.
This malpositioning can put pressure on the spinal cord, as well as the nerves that emanate from the spinal column. This pressure can lead to pain in the lower back and leg.
Spondylolisthesis of the lumbar region (meaning that it occurs in the lower back) is the most common. Specifically, the L5-S1 level of the spine is most frequently affected by spondylolisthesis, followed by the L4-5 level.
Is Spondylolisthesis The Same As a Slipped Disc?
You’ve probably heard the common medical term, “a slipped disc”. While this may seem to indicate the slippage involved in spondylolisthesis, it’s an entirely different condition.
Spondylolisthesis affects the spinal bones, which are known as vertebrae. A slipped disc is an injury involving an intervertebral disc, which is a cushion of shock-absorbing tissue. There’s an intervertebral disc located in between each of the vertebrae in the spine.
Given that spondylolisthesis and a slipped disc affect different parts of the spine and develop differently, it’s crucial to distinguish them. A spinal specialist can give you an accurate diagnosis of back pain.
Spondylolisthesis vs. Spondylolysis
As another spinal condition that’s commonly confused with spondylolisthesis, you may have heard of spondylolysis. This condition, unlike a slipped disc, is related to spondylolisthesis. However, they’re still different conditions.
Spondylolysis is a stress fracture that runs through the pars interarticularis, a small segment of bone that connects two vertebrae. When the pars interarticularis is fractured, patients may experience back pain that worsens with physical activity. However, not all spondylolysis patients have symptoms.
Approximately one out of 20 people have spondylolysis, making it a relatively common condition. Additionally, spondylolysis can lead to spondylolisthesis. This is because the pars interarticularis fracture can diminish the stability of the spine and potentially lead to slippage.
What Are The Most Common Causes of Spondylolisthesis?
Spondylolisthesis has several possible causes, the most common of which include:
- Spinal degeneration
The most common cause of spondylolisthesis is degenerative changes in the vertebral joints and cartilage due to aging. When spondylolisthesis is caused by age-related spinal changes, it’s known as degenerative spondylolisthesis.
- Birth defects
Younger individuals may experience spondylolisthesis caused by a birth defect in the facet of the vertebra. The defect, which is present at birth, can cause the vertebra to slip out of position. This is referred to as dysplastic spondylolisthesis.
- Spinal trauma
Spondylolisthesis can also result from sudden trauma, such as a sports injury or car accident. This is known as traumatic spondylolisthesis and can occur in people of all ages.
- Sports injury
In athletes that repetitively strain and overstretch the spine, spondylolisthesis is a relatively common injury. This is especially true in younger athletes, given that their spines haven’t fully developed.

Key Spondylolisthesis Symptoms
Lower Back Pain
The most frequent symptom of lumbar spondylolisthesis is lower back pain. The pain typically worsens after exercise and abates when you sit or bend forward.
Reduced Mobility
Decreased range of motion and tightness of the hamstring muscles are common spondylolisthesis symptoms.
Neurological Symptoms
The nerve compression may also result in pain, numbness, tingling, or weakness in the legs, and in cases of severe compression, loss of bowel or bladder control.
Spinal Stenosis
Spinal stenosis isn’t exactly a symptom of spondylolisthesis. However, degenerative spondylolisthesis is a prevalent cause of spinal stenosis, which is an abnormal narrowing of the spinal canal.
How Is Spondylolisthesis Diagnosed?
A physician specializing in spinal disorders can diagnose spondylolisthesis using radiographs and x-ray imaging, as well as a comprehensive physical exam. You’ll likely stand sideways as the x-rays are taken so your physician can see the vertebra’s slippage clearly.
After your physician has examined the imaging test results, the severity of your spondylolisthesis case will be graded. The grading scale is based on the degree of slippage from the vertebra’s normal position.
Upon making a diagnosis, a physician can recommend appropriate treatments for spondylolisthesis.
What Are Spondylolisthesis Grades?
As aforementioned, spinal specialists use a grading system to determine the severity of spondylolisthesis cases. Spondylolisthesis grades include:
- Grade I: 1% to 25% slippage
- Grade II: 26% to 50% slippage
- Grade III: 51% to 75% slippage
- Grade IV: 76% to 100% slippage
- Grade V or Spondyloptosis: Over 100% Slippage
What Makes Spondylolisthesis Worse?
Several factors can worsen spondylolisthesis, including:
- High-intensity physical activities
- Heavy lifting
- Poor posture
- Being involved in an auto accident
If you’ve been diagnosed with spondylolisthesis, your physician likely recommended lifestyle adjustments to help you avoid the factors listed above.
Spondylolisthesis Exercises To Avoid
Any exercises that involve heavy lifting and excessive twisting or bending should be avoided with spondylolisthesis. If you enjoy a specific sport, you should talk to your physician about whether it’s safe to participate in that sport while you’re struggling with spondylolisthesis symptoms.
Sports that tend to exacerbate spondylolisthesis symptoms include:
- Weightlifting and powerlifting
- Running
- Football
- Soccer
- Diving
- Competitive swimming
- Gymnastics
- Certain types of dance, including ballet
Spondylolisthesis Treatment
Treatments for spondylolisthesis include physical therapy, exercises for relieving pressure on the affected spinal nerves, medication, and epidural steroid injections. In many patients, these treatments are sufficient to alleviate the symptoms of spondylolisthesis.
What Does Physical Therapy For Spondylolisthesis Involve?
Physical therapists can help patients manage spondylolisthesis in several ways.
For one, your PT can offer valuable insights and education about how your lifestyle is affecting your symptoms. From your exercise regimen to your footwear to your posture, your physical therapist can identify areas for improvement. In making the recommended adjustments, you can likely reduce the pressure on your spine, leading to an improvement in spondylolisthesis symptoms.
Additionally, your PT can implement various non-invasive methods of pain management. Targeted heat and cold therapy can help alleviate inflammation and pain. Electrical stimulation is another popular method among physical therapists to gently reduce the transmission of pain signals to the brain.
Physical therapists can also recommend stretching and strengthening exercises for spondylolisthesis. By stretching to reduce muscle tension, you can gain greater back flexibility. By strengthening various muscle groups, you can gain greater stability in the lumbar spine, hips, and pelvis.
Does Chiropractic Care Help With Spondylolisthesis?
Many spondylolisthesis patients find that chiropractic care is a helpful tool for alleviating their symptoms. Chiropractors specialize in spinal manipulation to treat issues involving the musculoskeletal system.
Key goals of chiropractic care for spondylolisthesis include improving spinal mechanics, restoring spinal function, and improving posture. In achieving these goals, your chiropractor may alleviate compression on the spinal nerves, which often leads to reduced symptoms.
One of the main benefits of chiropractic care for spondylolisthesis is that it’s non-invasive. Chiropractors focus on methods including manual and instrument-assisted manipulation to adjust the spine, making it a safe back pain treatment option.
Which Medications Are Used To Treat Spondylolisthesis?
Physicians often recommend over-the-counter medications to help spondylolisthesis patients manage pain and inflammation. In more advanced cases that don’t improve with over-the-counter options, physicians may instead suggest prescription medications.
There are a few different types of drugs that may help with spondylolisthesis. The main types include:
- Analgesics
In simpler terms, analgesics are painkillers. These over-the-counter medications’ primary function is to relieve pain. The most common analgesic is acetaminophen, or Tylenol.
- NSAIDs (non-steroidal anti-inflammatory drugs)
NSAIDs alleviate inflammation along with pain. There are numerous over-the-counter NSAIDs, such as aspirin, Aleve, and Advil (ibuprofen), as well as prescription NSAIDs.
- Neuropathic agents
This type of prescription medication can be helpful for patients suffering from spondylolisthesis nerve pain. Neuropathic agents target nerve pain directly and can help with spondylolisthesis symptoms including tingling, numbness, and weakness.
Gabapentin and pregabalin (Lyrica) are two of the most commonly prescribed neuropathic agents for spondylolisthesis.
- Muscle relaxants
Some spondylolisthesis patients experience chronic back pain caused by muscle spasms in the back. In these cases, physicians may prescribe a muscle relaxant to stop the spasms. Soma, Flexeril, Baclofen, Tizanidine, and Robaxin are among the most widely prescribed muscle relaxants.
Will I Need Spondylolisthesis Surgery?
For patients with moderate to severe spondylolisthesis who don’t respond to conservative therapies, physicians may recommend spinal decompression surgery. The idea of undergoing surgery can be daunting, but note that most patients’ symptoms improve with non-surgical treatment.
If you and your physician determine that surgery is the right route of treatment, you’ll likely discuss the spinal decompression procedure.
What is Spinal Decompression?
Spinal decompression involves removing portions of the vertebrae that impinge on the spinal cord and nerve roots. There are several different approaches to spinal decompression, including laminectomy, foraminotomy, discectomy, and corpectomy. For spondylolisthesis, surgeons often opt for laminectomy.
Laminectomy involves removing some or all of the lamina. This is the small section of bone that covers the back of the spinal canal. By removing it, your surgeon can create more space for the spinal nerves and alleviate nerve impingement.
Spinal decompression can have a dramatic effect, relieving pain and other spondylolisthesis symptoms. However, removing portions of the lamina reduces the stability of the spinal column. So, after decompression surgery, spinal stability remains a key concern for spondylolisthesis patients.
This is why surgeons traditionally perform spinal fusion after spinal decompression.
What is Spinal Fusion?
Spinal fusion involves placing bone graft material in between the affected vertebrae. Then, screws and rods are implanted to secure the graft in place and provide additional stability.
In the period following spinal fusion surgery, the bone graft material will spur the permanent joining of the affected vertebrae. This prevents all movement between the fused vertebrae, which can prevent instability in spondylolisthesis patients.
Unfortunately, in stabilizing the vertebrae, spinal fusion eliminates the natural independent motion that gives the spine flexibility. This diminishes patients’ ability to carry out certain movements, namely those that require the bending or twisting of the spine. Fusion has also been shown to promote the deterioration of adjacent vertebrae.
Regain your mobility with Premia Spine! Contact us now
The TOPS™ System For Spondylolisthesis
In a seven-year study for patients with degenerative spondylolisthesis and lumbar spinal stenosis, the TOPS™ System maintained clinical improvement and stability. Additionally, in a five-year study of the TOPS™ System for 10 patients with degenerative spondylolisthesis and lumbar spinal stenosis, the clinical outcome scores “improved significantly across all scoring systems”. In this study, there were no failures at five years and no patients required revision surgery.
The TOPS™ device is approved for use in Europe and many other countries. In the United States, the FDA granted Premia Spine approval to begin an IDE investigation of the TOPS™ System.
TOPS™ Testimonials
Patient and surgeon testimonials are highly encouraging for the TOPS™ System as a spondylolisthesis treatment. Many patients note that they’re able to return to their favorite activities after the TOPS™ procedure, as it preserves spinal mobility.
We encourage anyone with persistent back problems to consult a physician who specializes in spinal disorders and learn about the latest available treatment options.