10 Years After Spinal Fusion: Studies and Research
The 10-year anniversary of a spinal fusion is a substantial milestone, and one that often symbolizes reclaimed mobility with freedom from debilitating pain. But for some, the 10-year post-op mark can open the floodgates to unanswered questions: How long will my spinal fusion last? Is my current back pain a sign of surgery failure?
At spinal fusion’s decade mark, the biomechanical shifts spurred by a fused segment can start to manifest in the rest of the spine. Whether you’re currently symptom-free (and hoping to stay that way) or experiencing new discomfort near the original surgical site, long-term data can offer insights into what to expect.
In this detailed patient guide, we analyze the latest studies to decipher between normal age-related pain and surgery-related warning signs. We’ll explore adjacent segment disease, 10-year fusion revision rates, and motion-preserving innovations that are shifting outlooks for patients looking to avoid the complications linked to fusion.

Success Rates, Quality of Life, Revision Surgery: The 10-Year Statistics
Spinal fusion success rates vary from study to study, although numbers drop after 10 years (primarily due to reoperation and adjacent segment disease).
- A Global Spine Journal study evaluating multilevel spinal fusion outcomes in elderly patients found that 44 to 69% of patients reported improved health-related quality of life.
- A 2020 prospective 10-year follow-up assessment for spinal fusions reported a 7.5% chance of revision surgery 10 years after the procedure.
- Patients reported quality of life at the 10-year mark that’s only slightly lower than healthy peers and notably higher than scoliosis patients who didn’t undergo spinal surgery.
- A prospective 10-year follow-up study in the North American Spine Society Journal found that the benefits of lumbar spinal fusion on pain, disability, and health-related quality of life (HRQOL) were partially lost, but still meaningful, after a decade.
- In this study, which included 683 fusion patients for various spinal disorders (degenerative spondylolisthesis, isthmic spondylolisthesis, spinal stenosis, degenerative disc disease, and deformity), 25% of patients had undergone revision surgery by 10 years, and adjacent segment disease was considered a major cause for lost fusion benefits.
How Many Years Does a Spinal Fusion Last?
Spinal fusion is intended to last for life as a permanent solution. Many spinal fusion patients experience improved pain and mobility for many years after the surgery, although hardware failure and recurring back pain are common problems that may require reoperation.
Why Does Pain Return After a Decade? Understanding ASD and Pseudoarthrosis
An estimated 8% to 40% of lumbar spine surgery patients experience recurring or difficult-to-manage leg and back pain. Adjacent segment disease (ASD) and pseudoarthrosis (failed fusion) are the two leading reasons why pain returns 10 years after spinal fusion.
- Adjacent segment disease results from increased biomechanical stress on the neighboring vertebrae.
- Pseudoarthrosis occurs when the vertebrae fail to fuse properly.
Adjacent Segment Disease (ASD)
By stopping all motion at the fused segment, spinal fusion causes a domino effect, significantly increasing mechanical stress, segmental motion, and intradiscal pressure at the segments above and below it. It also alters their biomechanics, forcing them to bend and twist more than usual. These biomechanical changes leave the adjacent segments vulnerable to accelerated degeneration.
A study published in The Journal of Bone & Joint Surgery reported a rate of 36.1% for clinical adjacent segment degeneration requiring surgery 10 years after spinal fusion, while a review in Clinical Spine Surgery found that between 2% to 4% of spinal fusion patients per year experience ASD.
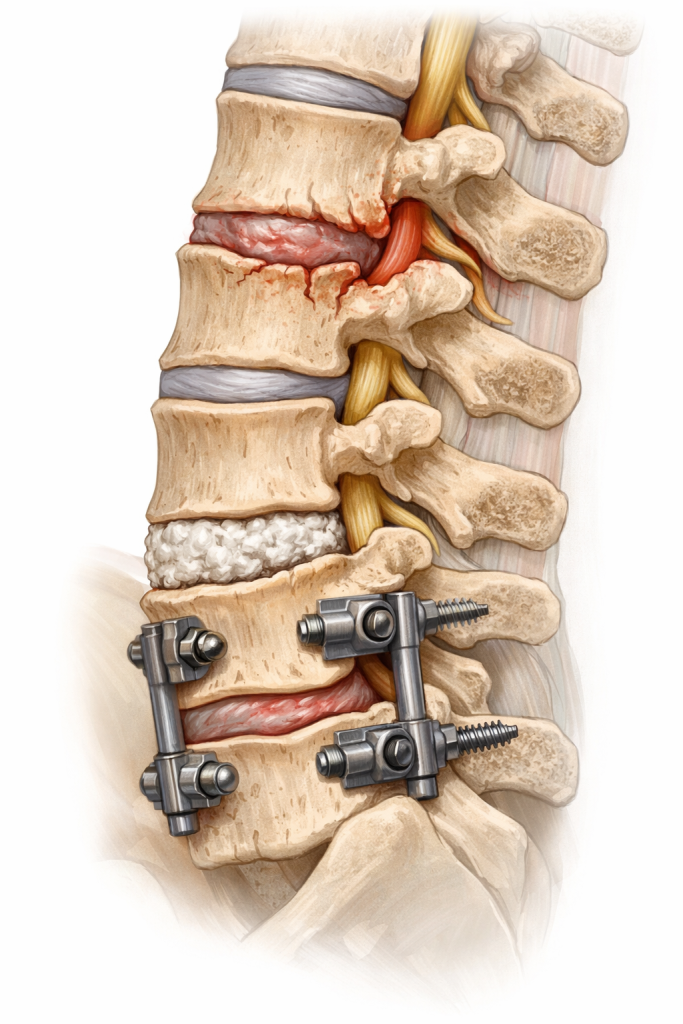
To prevent ASD after spinal fusion, consider these ASD risk factors:
- Being over age 60
- BMI over 25kg/m2
- History of smoking
- Pre-existing spinal degeneration
- Underlying medical conditions, including osteoporosis and rheumatoid arthritis
- Post-menopause stage
Pseudoarthrosis (Fusion Failure)
Pseudoarthrosis occurs when the vertebrae fail to merge into a single bone after spinal fusion. While some patients who develop this condition don’t experience symptoms (asymptomatic cases), it typically causes recurring lower back pain and neurological symptoms. Another spinal fusion procedure is the typical pseudoarthrosis treatment.
Pseudarthrosis rates after lumbar fusions vary, with rates ranging from 5% to 35%. A European Journal of Nuclear Medicine and Molecular Imaging study reported that pseudoarthrosis occurs in at least 15% of primary lumbar fusions. Older age, smoking, and a higher number of fused levels can increase your pseudarthrosis risk.
Signs Your Spinal Hardware Has Shifted or Failed
The pedicle screws, rods, spacers, cages, and other hardware used in spinal fusion may break, shift, or otherwise fail over time. Symptoms of post-fusion hardware failure include back pain, numbness, tingling, burning, spinal instability, reduced mobility, and crepitus (grinding, popping, or scraping). Hardware failure is more likely in cases of failed fusion.
Here’s the data on hardware failure after spinal fusion:
- Prevalence: A two-year Spine follow-up study of hardware failure in unconstrained lumbar pedicle screw systems reported a hardware failure rate of 22% and an overall fusion rate of 61%.
- A Journal of Neurosurgery study reported a symptomatic hardware failure rate of 20% after instrumented fusion for metastatic disease.
- Causes: A study published in The Spine Journal reported that screw fracture, one of the most common causes of hardware failure after lumbar fusion, has been shown to account for 34% of hardware failures.
- Location: A Journal of Spine Surgery study found that the sacroiliac joint is the most common site of long-term post-fusion hardware-related lower back pain.
Comparing Reoperation Rates for Fusion Approaches: ALIF vs. PLIF vs. TLIF vs. LLIF
A study published in The Journal of Neurosurgery found no differences in reoperation rates for symptomatic ASD between ALIF, PLIF, TLIF, and LLIF. However, possible complications do vary for these fusion approaches.
| Fusion Complications: ALIF vs. PLIF vs. TLIF vs. LLIF | ||||
| ALIF | PLIF | TLIF | LLIF | |
| Surgical Approach | Through the front (anterior) | Through the back (posterior) | Through the side of the spinal canal (from a midline incision in the back) | Through the side/flank (lateral) |
| Nerve Complication Risk | Low risk to spinal nerves; risk of injury to the sympathetic nervous system | Higher risk, requiring nerve root retraction | Moderate risk | Risk to the lumbar plexus (in the psoas muscle) |
| Vascular Complication Risk | Highest risk, requiring significant blood vessel retraction | Lower risk | Lower risk | Lower risk |
| Muscular Trauma Risk | Lower risk | Higher risk, requiring paraspinal muscle retraction | Moderate risk, with minimally invasive approaches available | Lower risk |
| Dural Tear Risk | Lower risk | Higher risk, requiring dural sac retraction | Moderate risk, requiring minimal dural sac retraction | Lower risk |
How to Tell The Difference Between Fusion Failure and Age-Related Spinal Changes
Differentiating between fusion failure and age-related spinal changes often requires imaging tests, including flexion/extension X-rays, CT scans, or MRIs, to pinpoint the location of the degeneration. Degeneration at the fused level or adjacent levels points to fusion failure, while degeneration at other spinal levels may stem from age-related changes.
Is Spinal Fusion a Disability? Navigating Disability Benefits at the Decade Mark
Spinal fusion may be considered a disability if the patient meets certain qualifications, including specific mobility restrictions, and qualifying patients can receive Social Security benefits.
To receive disability benefits after undergoing lumbar spinal fusion, patients must have been diagnosed with a disorder of the spine, such as:
- Spinal stenosis
- Spondylolisthesis
- Degenerative disc disease
- Vertebral fracture
- Osteoarthritis
- Any other spinal disorder that affects the spinal cord or nerve root
Here’s a checklist of the required information to file an Adult Disability Application with the Social Security Administration:
- Birthdate and place of birth
- Marriage and divorce information, if applicable
- Names and birth dates for any children who became disabled before age 22, are under age 18 and unmarried, or are aged 18 to 19 and attending secondary school full time
- U.S. military service information, if applicable, including the duty type and branch
- Employer name, employment start and end dates, and total wages for the current and past two years
- Self-employment details for the current and past two years, if applicable, including the business type and total net income
- Bank information for direct deposits, including the account type, number, and routing number
- Contact information for an alternate individual who understands your medical condition and can help with your claim
- Contact information for your doctors, healthcare providers, hospitals, and clinics
- Dates of exams, treatments, and medical tests, and the names of providers who sent them for you
- Patient ID numbers
- Names of all medications, both prescription and over-the-counter, including the prescribing doctor’s name and the reason for the medication
- Other relevant medical records (i.e. worker’s comp, vocational rehab, etc.)
- Job history, including the date your condition began impacting your work, the types of jobs you had before you became unable to work, and the types of duties you performed
- Education and training information
Social Security disability claims generally have a low approval rate, with an average final award rate of 31% for claims filed from 2010 through 2019. To improve your odds of success, make sure you submit a complete application with extensive supplementary information, and consider hiring a seasoned attorney who specializes in Social Security disability law.
Lifestyle Mastery: Staying Mobile at the 10-Year Mark
For most patients who undergo a single-level spinal fusion, mobility restrictions aren’t dramatically life-altering. Once the fused segment fully heals within six months to a year, these patients can often partake in their normal activities, though spinal bending, rotations, and stretches may be marginally limited. Patients who have multiple spinal levels fused are likely to experience significant mobility restrictions.
Staying active and adhering to your doctor’s guidance can help you stay mobile and pain-free beyond the 10-year mark.
Recommended Exercises (Swimming, Walking, Core)
Consider these forms of exercise as you work toward a long-term, post-fusion exercise routine:
- Swimming and water aerobics: Exercising in water takes the strain off your spine and other joints, allowing you to gain strength and stamina without the impact.
- Walking: Simple, accessible, and low-impact, walking can help preserve your mobility after fusion. Even taking short walks throughout the day can benefit your physical fitness and overall health.
- Gentle stretching and strengthening: Whether you complete them at home, at the gym, or even at the park on a sunny day, low-impact stretches and strengthening exercises can help alleviate impact on your spine. Talk to your PT for personalized recommendations that suit your stage of recovery, and take a look at our spinal stenosis exercise recommendations.
Activities to Avoid (Twisting, High-Impact)
Patients are typically advised against these forms of exercise after spinal fusion:
- Heavy weightlifting
- Activities involving repeated twisting, like golf
- Activities involving deep lower back bends, like gymnastics, diving, and certain yoga poses
- High-impact exercise, like running and contact sports
Supportive Equipment
As you navigate temporary and permanent restrictions after spinal fusion, specialized equipment can help you stay mobile, such as:
- Mobility aids, like canes and walkers, for stability while moving around the house during the early healing stages
- A reacher or grabber tool to retrieve items from the floor or high shelves and avoid bending or extending the spine
- Dressing sticks, sock aids, and shoe horns, which can help you get dressed without straining your spine
- Shower chairs and shower rails to provide stability in the shower when it may be difficult to stand after surgery
- A handheld showerhead can also be helpful post-fusion for bathing without significant bending or twisting.
- A raised toilet seat to prevent discomfort and lumbar spine impact while lowering yourself to the toilet
How to Overcome the Fear of Movement (Kinesiophobia)
A Frontiers in Neurology study found that 65.2% of lumbar fusion patients exhibit motor phobia, also known as kinesiophobia or fear of movement. Though understandable, kinesiophobia can ultimately harm your mobility and quality of life. Here are some expert-backed tips to overcome it:
- Seek support from a physical therapist, who can outline a safe, gradual return to movement.
- Talk to a therapist or counselor to overcome mental barriers to movement.
- Gain knowledge of your condition and the fusion procedure, learning how safe movements can help (not harm) the healing process.
- Set progressive, attainable movement goals to structure your return to exercise.
- Link movement to other enjoyable activities, like listening to music or socializing with friends.
- Implement other stress management techniques, like box breathing, meditation, mindfulness, and journaling.

Other Mental Health Challenges After Spinal Fusion
Ongoing pain, activity restrictions, and the inherent challenges of recovering from surgery can contribute to emotional and mental health challenges after spinal fusion. It’s a common issue: A 2024 study found that 23% of patients who underwent lumbar spine surgery reported psychological distress.
Along with following your surgeon’s recommendations and adopting healthy lifestyle habits, these tips can help your mental well-being after spinal surgery:
- Lean on loved ones for support and prioritize meaningful social interactions.
- Focus on getting high-quality sleep every night by creating a consistent sleep schedule, practicing good “sleep hygiene”, and finding a supportive, comfortable sleeping position.
- Consider talking to a therapist or counselor for professional mental health support as you navigate the post-fusion recovery process.
Red Flags: When to See a Surgeon 10+ Years Post-Op
If you experience any of these warning signs after spinal fusion, schedule an appointment with your surgeon to check for signs of failed fusion or recurring spinal issues:
- Severe, new, or worsening pain
- Tingling, weakness, or numbness
- Spinal instability
If you experience any of these red flag symptoms, seek emergency medical care, as they point to severe, possibly life-threatening neurological issues:
- Bladder or bowel dysfunction
- Sexual dysfunction
- Saddle anesthesia (numbness in the inner thighs, buttocks, and perineum)
- Progressive or severe leg weakness or numbness
The Path Forward: Motion-Preserving Fusion Alternatives
A lumbar fusion alternative is often a good choice for patients seeking to avoid recurring pain after spinal fusion. The TOPS System from Premia Spine is an FDA-approved option to correct lumbar spinal disorders while omitting the fusion process.

The TOPS System replaces the anatomical spinal structures removed in decompression surgery. For example, the facet joint or lamina may be removed during decompression to alleviate nerve impingement. Then, the TOPS System can be secured to the affected area to restore a stabilized range of motion.
Regain your mobility with Premia Spine! Contact us now
- Eliminate ASD risk: Since the TOPS System reestablishes motion in every direction, including extension, flexion, lateral bending, and axial rotation, patients aren’t subject to significant mobility restrictions after the procedure. This complete range of motion also removes the risk of adjacent segment disease and related complications.
- Improve quality of life: The TOPS System U.S. clinical study found that two years after surgery, 77% of TOPS patients achieved overall clinical success compared to 24% of fusion patients. This major contrast illustrates how TOPS can improve surgical outcomes, quality of life, and the overall treatment process for patients with lumbar spinal stenosis and spondylolisthesis.
- Confirmed superiority to fusion: TOPS’ superiority to fusion isn’t just indicated by clinical research: It’s been confirmed by the FDA. In addition to earning FDA approval for degenerative spondylolisthesis with lumbar spinal stenosis at one level from L3 to L5, the TOPS System was awarded a superior-to-fusion claim from the FDA. This achievement is a definitive seal of approval for patients seeking alternatives to lumbar fusion that won’t compromise their mobility or subject them to adjacent segment disease or other complications.
- Positive long-term outcomes: A five-year study published in World Neurosurgery found that the TOPS implant maintained motion and clinical improvement over the entire study period, with no patients requiring revision surgery. Patients treated with TOPS also showed significant improvements across all scoring systems, including radiographs, MRI scans, and back and leg pain scores, among others.
FAQ Section
- What to expect 10 years after spinal fusion?
Expect to have some limits on your spinal movements, particularly deep bends and twists. But if the fusion was successful, you’ll likely be able to lead a normal life with low-impact physical activity. You may eventually experience fusion complications, such as adjacent segment degeneration, hardware failure, or recurring pain.
- Can spinal fusion cause problems later in life?
Spinal fusion can cause problems later in life, mainly adjacent segment disease, hardware failure, recurrent pain, and limited mobility. Spinal fusion generally isn’t advised for younger patients for this reason – since they have several decades left to live, there’s more time for issues like adjacent level degeneration to develop.
- Does spinal fusion impact mental health?
Yes, spinal fusion can impact mental health, especially if it leads to ongoing pain and compromises your quality of life.
- How many years do spinal fusions last?
Spinal fusions are intended to last a lifetime, but failed fusion, hardware failure, adjacent segment disease, and other complications can lead to reoperation.
- Will I ever be normal after spinal fusion?
With proper aftercare, spinal fusion patients usually return to normal.