How Scoliosis Affects Life for Elderly People
Scoliosis is prevalent among children and teenagers. However, it can also have a large, far-reaching impact on the elderly population.
While scoliosis can develop with no apparent cause, it can also form as a result of age-related spinal degeneration. Although wear and tear on the spine is inevitable with age, it can diminish elderly individuals’ quality of life.
Here, we’ll discuss scoliosis, its impact on the elderly, and how scoliosis treatment with the innovative TOPS spinal implant can provide symptom relief.
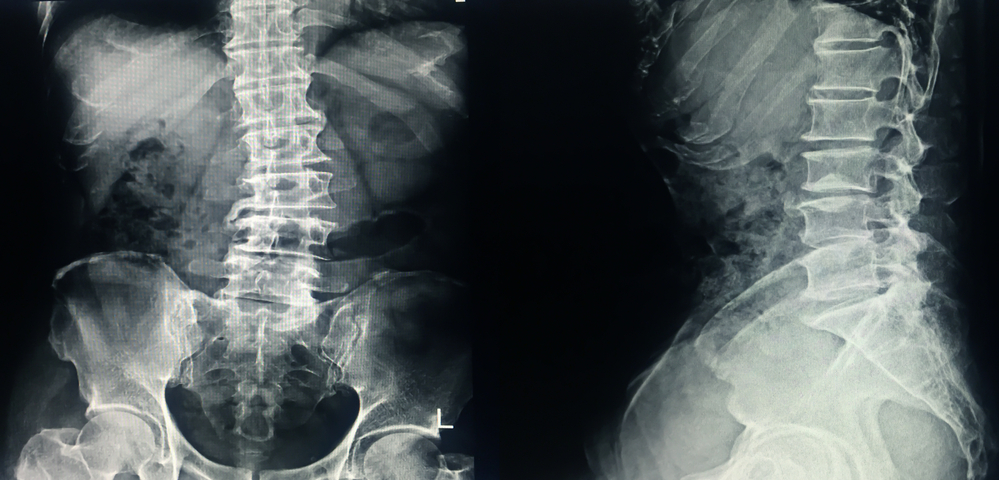
What is Scoliosis?
Scoliosis refers to an atypical sideways curvature of the spine. Usually, scoliosis appears in childhood or during adolescence.
The normal curvature of the spine is an S-shape when it’s seen from the side. With this curve, the neck (cervical spine) has a small forward curve, the upper/middle part of the back (thoracic spine) has an outward curve, and the lower back (lumbar spine) has an inward curve.
From the back, a spine with a normal curvature is straight. The vertebra, which are the bones of the spine, are stacked on top of each other. With scoliosis, some of the vertebrae curve sideways.
How is Scoliosis Diagnosed?
Most often, scoliosis is diagnosed in patients when they are aged between 10 and 15. Early diagnosis of this condition is ideal, as it allows physicians to implement scoliosis treatments while the body is still developing. In fact, with early intervention, it’s often possible to limit the progression of the abnormal spinal curve.
With that said, not all cases of scoliosis are diagnosed at a young age. Cases that are seen in adulthood can vary in cause.
What Causes Scoliosis in The Elderly?
Idiopathic Scoliosis
When scoliosis is idiopathic, it means that there’s no apparent cause for the abnormal spinal curve. This is the same type of scoliosis that’s often found in teenagers. Idiopathic scoliosis can begin during adolescence, but not cause symptoms until the patient is an adult.
In cases of idiopathic scoliosis, if the spinal curve is significant, it can become more severe over time. This can lead to adverse symptoms in adulthood.
However, cases of idiopathic scoliosis that don’t worsen can still lead to pain and other symptoms in adulthood. This is because the spinal asymmetry can gradually damage the patient’s spinal discs, muscles, and joints.
Degenerative Scoliosis
Degenerative scoliosis, which is also called adult-onset scoliosis, occurs as a result of spinal degeneration. With this type of scoliosis, the spinal wear and tear that naturally occurs with aging causes the spine to curve sideways.
Many cases of adult scoliosis are at least in part impacted by spinal degeneration. It triggers symmetry in the spine that gradually becomes worse as the patient ages. As degenerative scoliosis progresses, the facet joints and intervertebral discs that support the spine continually break down.
Degenerative scoliosis can be asymptomatic, especially in its early stages. However, if it does cause symptoms, patients may experience:
- A dull ache in the back
- Sciatica, which is pain that radiates from the lower back down one (or both) legs
- Back pain that’s exacerbating by standing for prolonged periods and gets better with rest
Traumatic Scoliosis
Traumatic scoliosis is a type of scoliosis that occurs after the spine is subject to a trauma, such as a car accident. The sudden trauma can create fractures in the spine, which may compromise spinal strength and alignment. This can result in scoliosis.
Scoliosis in The Elderly
While scoliosis is commonly thought to primarily affect teenagers, it has a large impact on the elderly.
In a study that measured the prevalence of scoliosis in adults between the ages of 60 and 90, 68% were found to have scoliosis.
Symptoms of adult scoliosis can be disabling, especially for elderly individuals. Examples of symptoms of severe scoliosis in the elderly include:
- Fatigue
- Shortness of breath
- Difficulty walking
- Difficulty standing straight
- Having the sensation of being full very soon while eating
- Bone spurs
Ultimately, scoliosis in the elderly can lead to reduced mobility, difficulty completing daily tasks, and chronic pain. Older adults with scoliosis may no longer be able to participate in activities that they used to enjoy.
A variety of treatment options can be implemented to help reduce the impact of scoliosis on an elderly patient’s day-to-day life. Physicians generally begin with non-surgical treatments, such as physical therapy and lifestyle modifications.
Exercises For Scoliosis in The Elderly
Targeted exercise for scoliosis in the elderly can help improve spinal flexibility and alignment. Examples of exercises that you can try include:
- Pelvic tilts
Lie on your back and bend your knees so that the soles of your feet lie flat on the ground. Contract your abdomen so that your pelvis tilts up to the ceiling, with your lower back flat against the ground. Hold it for 20 seconds, release, and repeat.
- Latissimus dorsi stretch
This stretch can support the lat muscles, which often become tense in patients with scoliosis. Stand up straight and place your hands above your head. Begin to bend at one side of your body, leaning gently until you feel a stretch along your side. Hold for 10 seconds, return to the original position, and repeat to the other side.
- Child’s pose
This yoga posture can help release tension in the back. Kneel on the floor, placing a blanket beneath your knees and shins if needed. Move your hips towards your heels, reach your arms forward, and place your hands flat on the floor. Breathe and relax in the stretch.
If non-surgical scoliosis treatment methods fail after several months, consider spinal surgery to improve scoliosis symptoms.
Spinal Surgery For Severe Scoliosis in The Elderly
For cases of degenerative scoliosis in the elderly, spinal decompression surgery is a viable treatment option.
Decompression surgery involves removing a portion of a spinal bone (vertebra) along with other spinal tissues, if needed. This relieves pain and sciatica symptoms caused by nerve compression.
By creating more space in the spinal canal, decompression surgery is often a successful treatment for degenerative scoliosis. It encourages the healing of damaged tissues while relieving pressure on nearby nerves.
Regain your mobility with Premia Spine! Contact us now
However, after decompression surgery, there’s a risk of spinal instability. So, this scoliosis treatment is generally paired with spinal fusion to restore spinal stability. The TOPS System is a spinal fusion alternative that can stabilize the spine without many of the downsides associated with fusion.
Spinal Fusion in Scoliosis Surgery
Spinal fusion is commonly completed at the same time as spinal decompression. It involves placing bone graft material in between two vertebrae in the treatment area. After the procedure, the bone graft will gradually cause the vertebrae to fuse into one bone.
By fusing the vertebrae, spinal fusion prevents spinal instability. However, it also prevents motion in the fused portion of the spine. Especially in elderly individuals, spinal fusion can diminish mobility and hold you back from participating in various activities.
Additionally, the healing process for spinal fusion requires the bone to heal. This makes for a lengthy, often painful recovery.
Spinal Implants
TOPS is a spinal arthroplasty system that replaces the spinal tissues that are removed during decompression surgery. Unlike spinal fusion, this mechanical implant device preserves the motion of the spine while preventing spinal instability.
After spinal decompression is performed, a surgeon can place the TOPS spinal implant into the targeted area. This system is designed for use between the segments L2 and L5 of the lumbar spine. Once implanted, the TOPS device controls the motion of the spine without inhibiting its flexibility.
Patients who undergo spinal decompression with the TOPS System for degenerative scoliosis can bend and twist the spine soon after the procedure. Additionally, the recovery process for decompression surgery with TOPS is much shorter than that of spinal fusion.
To learn more about the TOPS System in spinal decompression surgery for scoliosis treatment, contract Premia Spine today.